- About Us
- Causes of Infertility
- Fertility Treatments
- Basic Infertility Therapy
- Surgical Procedures
- Ovulation Drugs
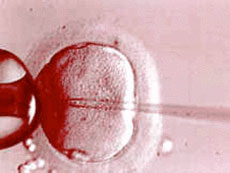
- In Vitro Fertilization Overview
- Donor Egg
- Surrogacy
- Preimplantation Genetic Screening
- Egg Freezing
- Frozen Embryo Transfer (FET)
- Recurrent Miscarriage
- Single Mothers by Choice
- LGBTQIA+
- Tubal Reversal
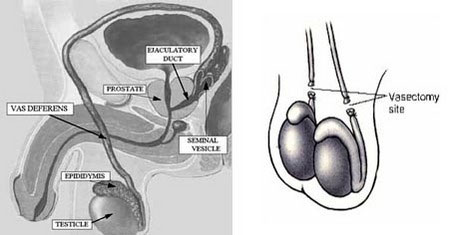
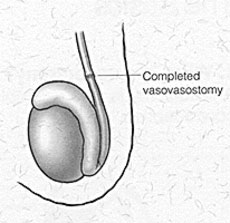
- Vasectomy Reversal
- Schedule Appointment
- Affording Treatment
- Support Group
- Lab Services
- Medication Instructions
- Contact Us